Transcranial Magnetic Stimulation
Transcranial magnetic stimulation (TMS) is a non-invasive and relatively safe technology where electromagnetic currents in a coil produces magnetic pulses which crosses the cranium and induces neuron depolarization (Defrin et al. 2007). Magnetic stimulation of the motor cortex has been shown to attenuate post-stroke pain (Migita et al. 1995).
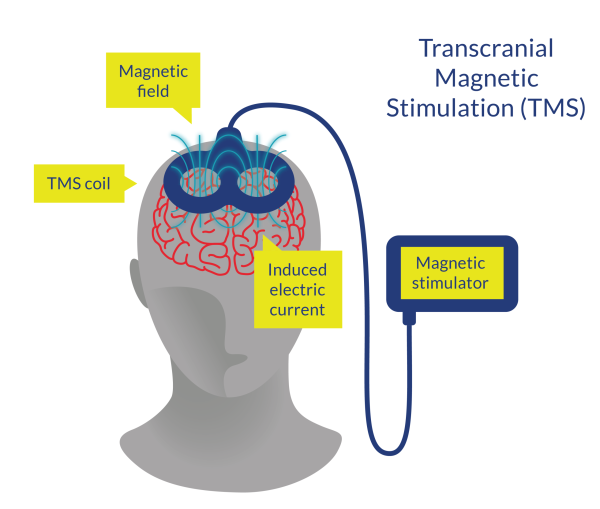
Figure 2. Transcranial Magnetic Stimulation (TMS)
Discussion
There is conflicting evidence for the effectiveness of rTMS in reducing pain post SCI. Three RCTs found no significant difference between rTMS and sham groups in pain intensity post intervention (Defrin et al. 2017; Kange et al. 2009; Ylimaz et al. 2014). Two RCTs found rTMS significantly reduced pain intensity compared to a sham control treatment (Jette et al. 2013; Nardone et al. 2017). Jette et al. (2013) found that reduction in pain intensity was greater among those incomplete injury compared to complete. Evaluation of potential subgroups that may benefit from rTMS treatment is warranted.
Conclusion
There is level 1a evidence (from four RCTs: Jette et al. 2013; Defrin et al. 2007; ) that rTMS may not significantly reduce average pain intensity post-SCI.
There is level 1b evidence (from one RCT: Kang et al. 2009) that rTMS significantly reduces worst pain compared to sham rTMS.
